Cardiology Module 4
Quiz Summary
0 of 35 Questions completed
Questions:
Information
You have already completed the quiz before. Hence you can not start it again.
Quiz is loading…
You must sign in or sign up to start the quiz.
You must first complete the following:
Results
Results
0 of 35 Questions answered correctly
Your time:
Time has elapsed
You have reached 0 of 0 point(s), (0)
Earned Point(s): 0 of 0, (0)
0 Essay(s) Pending (Possible Point(s): 0)
| Average score |
|
| Your score |
|
Categories
- Not categorized 0%
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- Current
- Review
- Answered
- Correct
- Incorrect
-
Question 1 of 35
1. Question
Which of the following cardiac mechanisms primarily contributes to the development of right ventricular failure?
CorrectIncorrect -
Question 2 of 35
2. Question
Based on the findings from the recent REDUCE-AMI trial, which of the following best reflects the management of heart failure with preserved ejection fraction (HFpEF) in post-myocardial infarction (MI) patients?
CorrectIncorrect -
Question 3 of 35
3. Question
A 58-year-old man with a history of hypertension and type 2 diabetes presents to the clinic complaining of intermittent chest pain, mostly occurring during exertion. His physical examination is unremarkable, and his resting electrocardiogram shows nonspecific ST-T wave changes.
He is able to walk two flights of stairs without angina or dyspnea. You are considering further testing to assess for coronary artery disease.
Which of the following is the most appropriate next step in the management of this patient?
CorrectIncorrect -
Question 4 of 35
4. Question
Which of the following is NOT an indication for permanent pacemaker insertion?
CorrectIncorrect -
Question 5 of 35
5. Question
Which of the following is an indication for permanent pacemaker insertion following an ST elevation myocardial infarction?
CorrectIncorrect -
Question 6 of 35
6. Question
Which of the following is less likely to occur following cardiac resynchronization therapy (CRT)?
CorrectIncorrect -
Question 7 of 35
7. Question
What would be the main reason for using troponin T and troponin I as the preferred biomarkers for myocardial injury?
CorrectIncorrect -
Question 8 of 35
8. Question
Which of the following is the most common acquired valve disease in Australasian patients aged over 75 years?
CorrectIncorrect -
Question 9 of 35
9. Question
A 72-year-old man with a background of coronary artery disease, hyperlipidemia and type 2 diabetes mellitus presents with symptoms of increasing fatigue and dyspnea for the last several months to a year.
Most recently, he noticed that he is increasingly becoming short of breath and fatigue just walking from across a room of less than 50 meters and is only comfortable at rest.
His current medications include aspirin, carvedilol, cilazapril, digoxin, spironolactone, furosemide, simvastatin, and glipizide.
On examination, his blood pressure is 95/60 mm Hg, pulse is 57/min, and respiration rate is 12/min. Cardiovascular examination reveals a displaced apex beat. Rhythm is regular and bradycardic. S1 and S2 are normal, with a grade 3/6 pan-systolic murmur at the apex. An S3 is present. There is no hepatojugular reflux. The lungs are clear. There is no ascites. The liver edge is palpable 1 cm below the right costal margin. The lower extremities are warm with decreased distal pulses bilaterally. There is no ankle edema.
Electrocardiogram shows sinus rhythm with a rate of 55/min. PR interval is 180 msec, QRS width is 180 msec, and QT interval is 380 msec. Left bundle branch block is seen.
A dobutamine stress echocardiogram reveals a left ventricular ejection fraction of 33% with a large anteroapical area of akinesis and no ischemia.
Which of the following is the most appropriate management option for this patient?
CorrectIncorrect -
Question 10 of 35
10. Question
What is the mechanism of action of aspirin?
CorrectIncorrect -
Question 11 of 35
11. Question
What is the mechanism of action of clopidogrel?
CorrectIncorrect -
Question 12 of 35
12. Question
What is the mechanism of action of Fondaparinux?
CorrectIncorrect -
Question 13 of 35
13. Question
What is the mechanism of action of enoxaparin(LMWH)?
CorrectIncorrect -
Question 14 of 35
14. Question
In patients with systolic LV dysfunction, which medication should be started regardless if patient is symptomatic or not?
CorrectIncorrect -
Question 15 of 35
15. Question
What is the mechanism of action of carvedilol?
CorrectIncorrect -
Question 16 of 35
16. Question
A patient presents with sudden onset severe retrosternal chest pain associated with shortness of breath and diaphoresis. ECG shows 2mm ST elevation over lead V1 and V2.
Which myocardial wall is the most likely to be affected?CorrectIncorrect -
Question 17 of 35
17. Question
What is the most likely diagnosis?
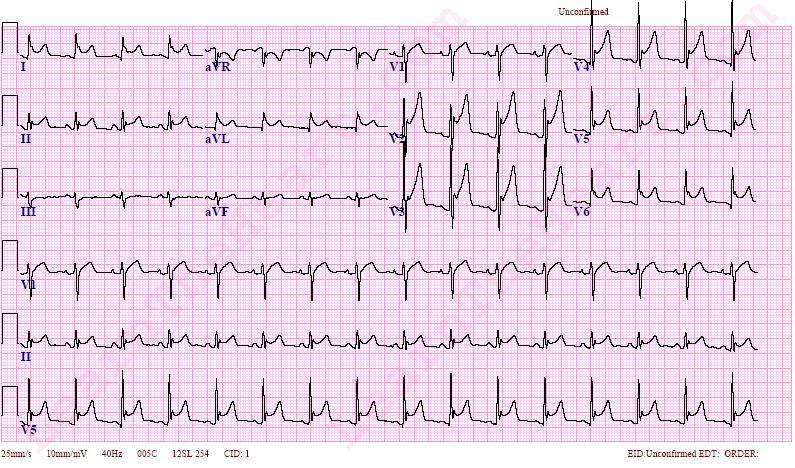 CorrectIncorrect
CorrectIncorrect -
Question 18 of 35
18. Question
What is the most likely diagnosis?
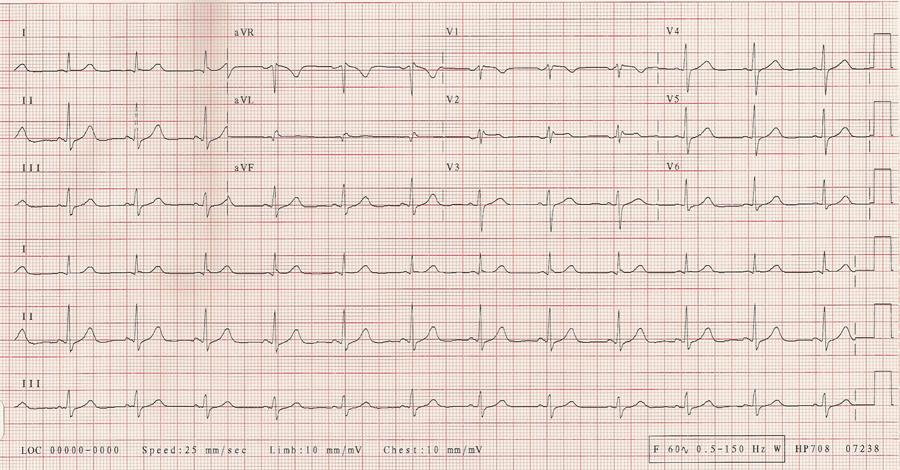 CorrectIncorrect
CorrectIncorrect -
Question 19 of 35
19. Question
An 18-year-old woman is evaluated for recurrent syncope. She has experienced four syncopal episodes in her lifetime, all of which occurred during activity. The most recent was last week, when she dove into a pool and had a brief loss of consciousness. Episodes have no prodrome, and she has had no dizziness.
She is healthy and active, without cardiopulmonary complaints, and takes no medications. Her maternal cousin drowned at age 10 years, and her mother has been diagnosed with a seizure disorder.
On physical examination, her blood pressure is 112/65 mm Hg and her pulse is 67/min and regular. The cardiopulmonary and general physical examinations are normal.
Her electrocardiogram is shown below:
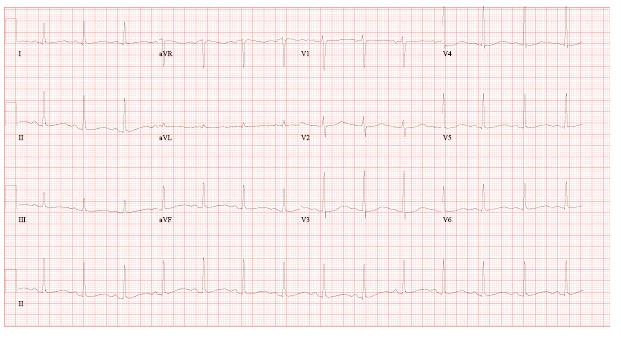
Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 20 of 35
20. Question
Which of the following medication should be avoided in this rhythm?
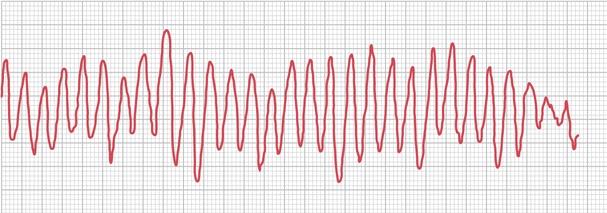 CorrectIncorrect
CorrectIncorrect -
Question 21 of 35
21. Question
In a patient who presents with this ECG finding, where is the most likely location of the block?
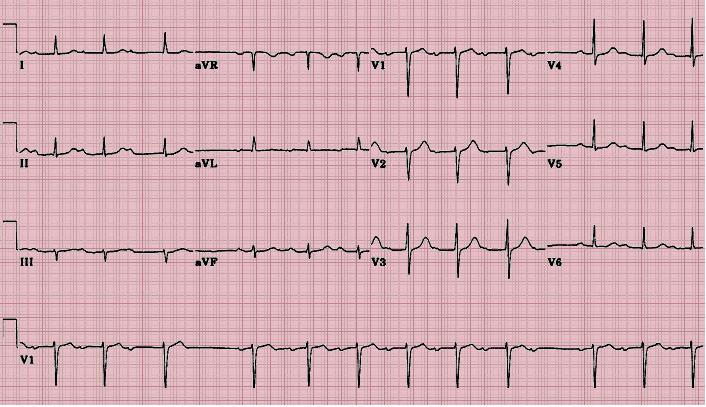 CorrectIncorrect
CorrectIncorrect -
Question 22 of 35
22. Question
A 65 year old lady presents with 3 episodes of syncope over the last 5 months.Each episode has been associated with exertion and has been preceded by palpitations.Episodes of syncope has been brief only lasting a few seconds.No urinary incontinence.No tongue biting. Holter monitor was reported as normal. Her ECG shows normal sinus rhythm with a right bundle branch block.
Which of the following is the most appropriate investigation?CorrectIncorrect -
Question 23 of 35
23. Question
A 50 year old man presents to his GP with atypical chest pain. He has a background of hypertension but is otherwise well with no other cardiac risk factors. Resting ECG shows left bundle branch block.
What is the most appropriate step?
CorrectIncorrect -
Question 24 of 35
24. Question
Which of the following contributes the greatest population attributes risk for myocardial infarction?
CorrectIncorrect -
Question 25 of 35
25. Question
If a patient presents to hospital with chest pain and has the following ECG, which ECG feature would predict the highest risk of in-hospital mortality?
CorrectIncorrect -
Question 26 of 35
26. Question
The following constitutes a positive stress ECG except?
CorrectIncorrect -
Question 27 of 35
27. Question
The following are indications for exercise stress ECG except?
CorrectIncorrect -
Question 28 of 35
28. Question
A 22-year-old man collapses immediately after being hit in the chest with a ball while playing lacrosse. Emergency medical personnel were present during the game and noted the initial rhythm to be ventricular fibrillation.
The patient underwent prompt defibrillation within 3 min, and normal sinus rhythm was restored.
The patient has been transported to the emergency room and is stable with a blood pressure of 128/76 mmHg and heart rate of 112 beats/min.
He has no prior history of syncope and no family history of sudden cardiac death. His electrocardiogram (ECG) is normal. There is no evidence of broken ribs or sternum by x-ray.
What is the most likely diagnosis?
CorrectIncorrect -
Question 29 of 35
29. Question
All of the following statements regarding sudden cardiac death are true except?
CorrectIncorrect -
Question 30 of 35
30. Question
The loss-of-function single nucleotide polymorphism of cytochrome P450 family 2 subfamily C member 19 enzyme (CYP2C19) would render this medication to be ineffective:
CorrectIncorrect -
Question 31 of 35
31. Question
Among patients with heart failure and a reduced ejection fraction, which of the following medication has been shown to reduce the risk of worsening heart failure?
CorrectIncorrect -
Question 32 of 35
32. Question
A 60 year old man with a background of advanced renal cell cancer presents with symptoms of chest pain and dyspnea, 20 days after receiving his first cycle of combination ipilimumab/nivolumab therapy.
Clinically, he appeared to be in gross fluid overload and was hypotensive. Chest x-ray shows cardiomegaly with interstitial edema. He had non-specific ST changes on ECG with a raised Hs-troponin T of 500.
Echocardiogram shows moderate to severe LV dysfunction with an estimated LV ejection fraction of 35 percent but with no regional wall motion abnormalities.
Which of the following would be the most appropriate next step?
CorrectIncorrect -
Question 33 of 35
33. Question
In patients with stable angina who are not on regular anti-anginal medications, what is the likely benefit of percutaneous coronary intervention (PCI) on the daily number of angina episodes?
CorrectIncorrect -
Question 34 of 35
34. Question
A 16-year-old teenager is referred for hypertension noted during a routine physical examination. The blood pressure in the upper limbs is significantly higher than in the lower limbs. A murmur is heard on the left back and inter-scapular area.
What is the most likely diagnosis?
CorrectIncorrect -
Question 35 of 35
35. Question
A child with a congenital heart defect presents with chronic hypoxia. As a compensatory mechanism, the body responds by increasing the production of red blood cells. This response is known as secondary erythrocytosis.
Which of the following best explains the underlying physiological process leading to this condition?
CorrectIncorrect
